Ultrasound Obstet Gynecol 2010; 35: 620–623
Published online in Wiley InterScience (www.interscience.wiley.com).
Letters to the Editor
Intra-amniotic N-terminal pro-brain natriuretic
peptide in severe twin-to-twin transfusion
syndrome treated by fetoscopic laser coagulation
Twin-to-twin transfusion syndrome (TTTS) is caused by unbalanced blood flow through intertwin vascular placental anastomoses and usually presents with oligo-hydramnios in the donor twin and polyoligo-hydramnios in the recipient1. A randomized controlled trial demon-strated that laser coagulation of placental anastomoses improves survival rate and lowers the rate of neuro-logical handicap2. The main cause of recipient death is cardiac overload disease as a consequence of hyper-volemia and systemic arterial hypertension3,4. The NH
2 (amino)-terminal fragment of pro-brain natriuretic pep-tide (NT-proBNP) is a neurohormone that is synthesized mainly in the cardiomyocytes of the ventricles in response to pressure overload, volume overload or myocardial damage. Bajoria et al. established that, in TTTS, fetal plasma BNP was correlated with cardiac function in the recipient5 and that the amount of amniotic BNP was increased in the recipient pocket6. Our objective was to investigate whether the concentration of NT-proBNP in the amniotic fluid of the recipient twin would be useful for predicting perinatal outcome, includ-ing survival and the occurrence of sequelae of cardiac overload disease, in cases of TTTS undergoing treatment by laser coagulation. The ability to predict fetal out-come would be useful for parental counseling and could influence clinical management, for example by indicat-ing selective feticide when fetal demise appears clearly unavoidable.
Amniotic fluid samples were collected from the recipient sac at the start of the fetoscopic procedure in 40 consec-utive cases of TTTS undergoing laser treatment (Stage I, n= 2; Stage II, n = 21; Stage III, n = 14; Stage IV,
n= 3). The concentration of NT-proBNP was measured
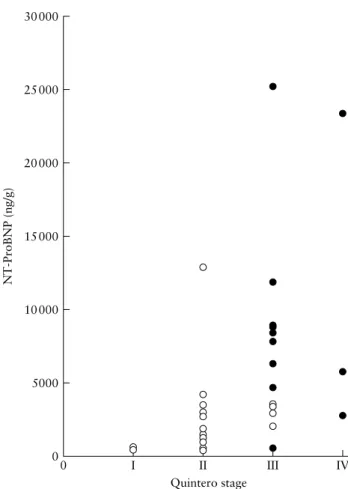
by electrochemiluminescence (Modular E170; Roche Diagnostics, Meylan, France) and, due to the matrix effect, reliable readings were obtained in 34 out of 40 cases (four missing values for Stage II and two missing values for Stage III cases). Concentrations of this marker were ana-lyzed in relation to the total concentration of amniotic proteins to correct for dilution associated with polyhy-dramnios (Modular P; Roche Diagnostics). The overall survival rate was 77%, with at least one survivor in 86% of cases. Five neonates (recipients) presented sequelae induced by cardiac overload (pulmonary stenosis and/or hypertrophic cardiomyopathy or pulmonary hyperten-sion). None developed subsequent complications. We observed a correlation between the amniotic concentra-tion of NT-proBNP and severity of TTTS, according to Quintero staging (P= 0.01) (Figure 1). No correlation
0 0 5000 10000 15000 NT-ProBNP (ng/g) 20000 25000 30000 I II Quintero stage III IV
Figure 1 Plot showing correlation between amniotic concentration of N-terminal pro-brain natriuretic peptide (NT-proBNP) and Quintero staging (
°
, no Doppler anomaly in recipient;ž
, presence of Doppler anomalies in recipient). There were seven overlapping values for NT-ProBNP, all below 5000 ng/g, for Stage II cases.was demonstrated between the amniotic concentrations of NT-proBNP and overall survival rate 48 h after laser coagulation (P= 0.6), at birth (P = 0.07) or at discharge (P= 0.2), recipient survival rate at discharge (P = 0.7), or occurrence of cardiac sequelae at birth in surviving recipients (P= 0.2).
It has been suggested in the literature that the amniotic concentration of NT-proBNP could be influenced by renal function7,8 and amniotic distension6,9. However, we observed no correlation between the amniotic concentrations of NT-proBNP and the deepest vertical amniotic fluid pocket, and so consider that alterations in NT-proBNP concentrations were mainly a result of cardiac overload. Some investigators have demonstrated that cardiac dysfunction in the recipient twin usually normalizes within 1 month after laser treatment10. Therefore, fetal outcome could be at least partially independent from the severity of fetal blood flow imbalance, as described by Quintero staging or any other cardiac parameter, at the time of laser treatment.
Letters to the Editor 621
In conclusion, we have demonstrated that the concen-tration of NT-proBNP in the amniotic fluid of the recipient was correlated with the severity of TTTS according to Quintero staging but did not predict perinatal outcome after laser coagulation treatment.
Acknowledgments
We would like to thank Siemensand Roche Diagnostics for the generous gifts of the cystatin C,β2-microglobulin and NT-proBNP assays.
A. Delabaere†‡, G. Marceau‡§, S. Kemeny‡§, V. Sapin‡§, S. Ughetto¶, K. Coste‡**and D. Gallot*†‡ †Fetal Maternal Medicine Unit and **Department of
Pediatrics, CHU Clermont-Ferrand, Maternit´e H ˆotel-Dieu, Boulevard L´eon Malfreyt, 63003 Clermont-Ferrand, ‡UMR CNRS 6247 GReD, Clermont Universit´e, Facult´e de M´edecine, §Department of Biochemistry and ¶Department of Biostatistics, CHU Clermont-Ferrand, 63000 Clermont-Ferrand, France *Correspondence. (e-mail: dgallot@chu-clermontferrand.fr)
DOI: 10.1002/uog.7579
References
1. Ville Y. Monochorionic twin pregnancies: ‘les liaisons dan-gereuses’. Ultrasound Obstet Gynecol 1997; 10: 82–85. 2. Senat M, Deprest J, Boulvain M, Paupe A, Winer N, Ville Y.
Endoscopic laser surgery versus serial amnioreduction for severe twin-to-twin transfusion syndrome. N Engl J Med 2004; 351: 136–144.
3. Mahieu-Caputo D, Dommergues M, Delezoide A, Lacoste M, Cai Y, Narcy F, Jolly D, Gonzales M, Dumez Y, Gubler M. Twin-to-twin transfusion syndrome. Role of the fetal renin-angiotensin system. Am J Pathol 2000; 156: 629–636. 4. Mahieu-Caputo D, Muller F, Joly D, Gubler M, Lebidois J,
Fermont L, Dumez Y, Dommergues M. Pathogenesis of twin-twin transfusion syndrome: the renin-angiotensin system hypothesis. Fetal Diagn Ther 2001; 16: 241–244.
5. Bajoria R, Ward S, Chatterjee R. Natriuretic peptides in the pathogenesis of cardiac dysfunction in the recipient fetus of twin-twin transfusion syndrome. Am J Obstet Gynecol 2002; 186: 121–127.
6. Bajoria R, Ward S, Chatterjee R. Brain natriuretic peptide and endothelin-1 in the pathogenesis of polyhydramnios-oligohydramnios in monochorionic twins. Am J Obstet Gynecol 2003; 189: 189–194.
7. Michielsen E, Bakker J, Kimmenade R, Pinto Y, Dieijen-Visser M. The diagnostic value of serum and urinary NT-proBNP for heart failure. Ann Clin Biochem 2008; 45: 389–394.
8. Linssen G, Damman K, Hillege H, Navis G, van Veldhuisen D, Voors A. Urinary N-terminal prohormone brain natriuretic peptide excretion in patients with chronic heart failure. Circulation 2009; 120: 35–41.
9. Carvajal J, Delpiano A, Cuello M, Poblete J, Casanello P, Sobrevia L, Weiner C. Brain natriuretic peptide (BNP) pro-duced by the human chorioamnion may mediate pregnancy myometrial quiescence. Reprod Sci 2009; 16: 32–42.
10. Van Mieghem T, Klaritsch P, Done E, Gucciardo L, Lewi P, Verhaeghe J, Lewi L, Deprest J. Assessment of fetal car-diac function before and after therapy for twin-to-twin transfusion syndrome. Am J Obstet Gynecol 2009; 200: 400.e1–7.
Rare case of postpartum hemorrhage caused by
rupture of a uterine artery pseudoaneurysm 3
months after Cesarean delivery
When postpartum hemorrhage occurs it is usually immedi-ately following or several hours or days after delivery, and it almost always takes place within 6 weeks1,2. Rupture of a uterine artery pseudoaneurysm subsequent to a Cesarean section is a rare cause of postpartum hemorrhage3,4, and delayed postpartum hemorrhage from a pseudoaneurysm may be misdiagnosed as hypermenorrhea. Here we present an extremely rare case of massive postpartum hemorrhage 3 months after a Cesarean section that was success-fully treated using selective uterine artery embolization (UAE).
A 24-year-old woman, gravida 1, para 1, delivered a healthy infant via emergency Cesarean section at a local clinic in October 2007. Arterial hemorrhaging from the left lower uterine incision occurred during the operation and the artery was ligated with silk thread immediately and completely. The patient’s postopera-tive and postpartum course was unremarkable, with the first menstruation in early December. On January 4, 2008, she was admitted to the same clinic with massive and continuous vaginal bleeding and received blood transfusions for shock. Since the bleeding stopped spontaneously after 5 days, she was diagnosed with hyper-menorrhea and prescribed low-dose contraceptive pills. However, massive vaginal bleeding started again on February 1, and she was transported by ambulance to our hospital on February 5 with persistent hemorrhag-ing.
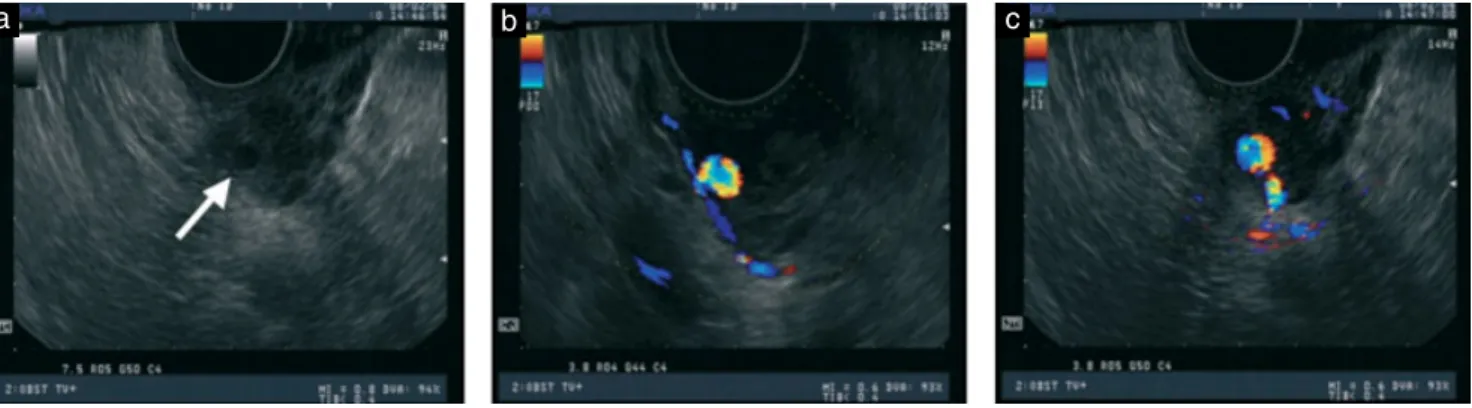
Examination revealed hypotension, tachycardia and anemia. B-mode and color Doppler ultrasonography showed a cystic lesion in the left wall of the lower uterus (Figure 1a) but no retained placental fragments or pathological findings in the uterine cavity. Longitudinal color Doppler ultrasonography showed a blood-filled cystic structure with mosaic flow pattern (Figures 1b and c). After administration of intravenous fluids and four units of red blood cell concentrate, three-dimensional computed tomography (3D-CT) with an intravenous contrast agent showed a 2-cm enhanced lesion in the left parauterine region with a surrounding low-density area consistent with a pseudoaneurysm. Angiograms, with access through the right femoral artery, revealed focal extravasation from a branch of the left uterine artery (Figure 2), and this artery was successfully embolized using absorbable gelatin sponge pledgets (Gelfoam, Pfizer Inc., New York, NY, USA).
The patient experienced minimal vaginal bleeding during the following 3 days and was discharged 1 week after the procedure. Normal menstruation resumed after 3 months, with normal 3D-CT scan results obtained at the 3-month follow-up visit.
Pseudoaneurysms can be detected using Doppler ultrasound, appearing as blood-filled cystic structures5.
622 Letters to the Editor
Figure 1 Ultrasonographic findings on admission: gray-scale ultrasound image showing a cystic lesion (arrow) in the lower left wall of the uterus (a) and color Doppler ultrasound images showing turbulent arterial flow within the cystic lesion in the longitudinal (b) and transverse (c) views. Note the presence of the parent artery in (c).
Figure 2 Non-selective pelvic arteriography showing a pseudoaneurysm (arrow) at the branch of the left uterine artery (a), superselective angiogram obtained using a microcatheter in the branch revealing a 2-cm pseudoaneurysm (arrow) (b) and late-phase internal iliac artery angiogram taken post-embolization showing complete occlusion of the left uterine artery and the pseudoaneurysm (c).
Duplex Doppler ultrasound shows turbulent arterial flow, while color Doppler imaging shows arterial flow swirling in different directions and at different velocities within the pseudoaneurysm, with colors varying according to the degree of turbulence6.
Arterial embolization has been used successfully in the management of postoperative, postabortion and postpartum intractable bleeding7. Advantages include high (90–95%) success rates, low complication rates, no surgical risks and preservation of fertility8.
In conclusion, in this case we found color Doppler ultrasonography to be useful in diagnosing a uterine artery pseudoaneurysm as the cause of a late postpartum hemorrhage, which was treated successfully by UAE. Thus, when a pseudoaneurysm is suspected following color Doppler ultrasound and a subsequent CT scan, angiography and UAE are recommended.
E. Hayata*, H. Matsuda and K. Furuya
Department of Obstetrics and Gynecology, National Defense Medical College, 3-2 Namiki, Tokorozawa, Saitama, 359-8513, Japan *Correspondence. (e-mail: e hayata@hotmail.com; hmatsuda@ndmc.ac.jp)
DOI: 10.1002/uog.7607
References
1. Jan H, Mehra G, Kent A. Postpartum hemorrhage due to a pseudo-aneurysm formation following cesarean delivery. Int J Gynaecol Obstet 2007; 98: 263–264.
2. Bromley PJ, Clark T, Weir IH, Zwirewich CV. Radiologic diag-nosis and management of uterine artery pseudoaneurysm: case report. Can Assoc Radiol J 1997; 48: 119–122.
3. Zimon AE, Hwang JK, Principe DL, Bahado-Singh RO. Pseu-doaneurysm of the uterine artery. Obstet Gynecol 1999; 94: 827–830.
Letters to the Editor 623
4. Pelage JP, Soyer P, Repiquet D, Herbreteau D, Le Dref O, Houdart E, Jacob D, Kardache M, Schurando P, Truc JB, Rymer R. Secondary postpartum hemorrhage: treatment with selective arterial embolization. Radiology 1999; 212: 385–389.
5. Langer JE, Cope C. Ultrasonographic diagnosis of uterine artery pseudoaneurysm after hysterectomy. J Ultrasound Med 1999; 18: 711–714.
6. Ball RH, Picus D, Goyal RK, Wilson DB, Rader JS. Ovarian
artery pseudoaneurysm: diagnosis by Doppler sonography and treatment with transcatheter embolization. J Ultrasound Med 1995; 14: 250–252.
7. Hennerici M, Neuerburg-Heusler D. Peripheral arteries. In Vascular diagnosis with ultrasound, Hennerici M, Neuerburg-Heusler D (eds). Thieme: New York, NY, 1998; 133–187. 8. Nowak D. Embolization materials. In Interventional Radiology,
Dondelinger RF, Rossi P, Kurdziel JC, Wallace S (eds). Thieme: New York, NY, 1990; 295–313.