The role of interventional pain management in chronic pain
7
0
0
Texte intégral
Figure
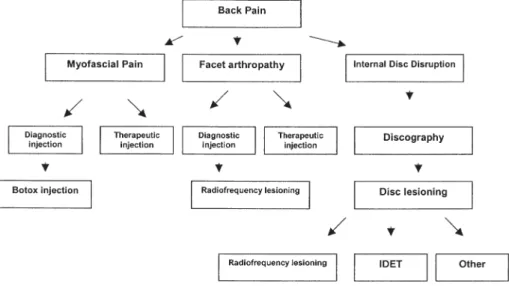
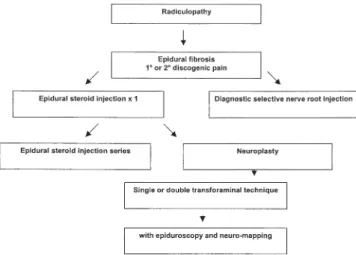


Documents relatifs