Recruitment, use, and satisfaction with a web platform supporting families of children with suspected or diagnosed developmental coordination disorder: A randomized feasibility trial
Texte intégral
Figure

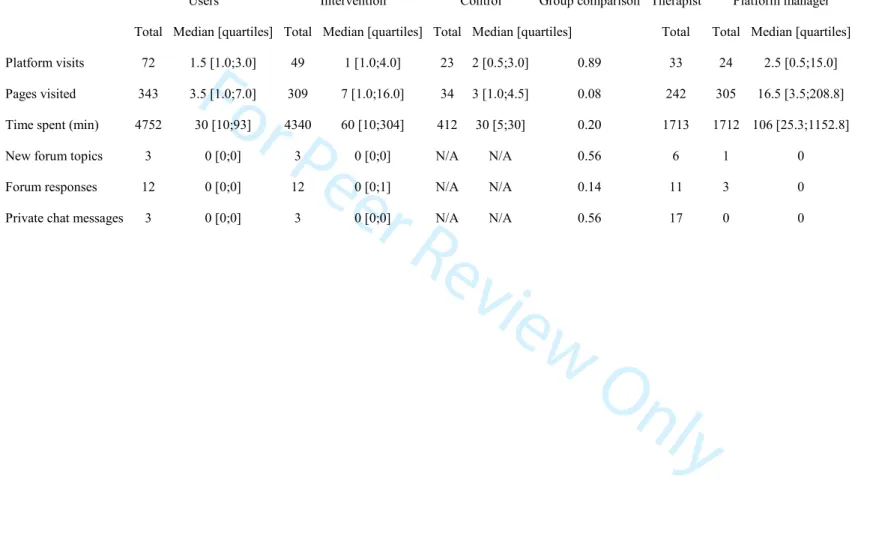
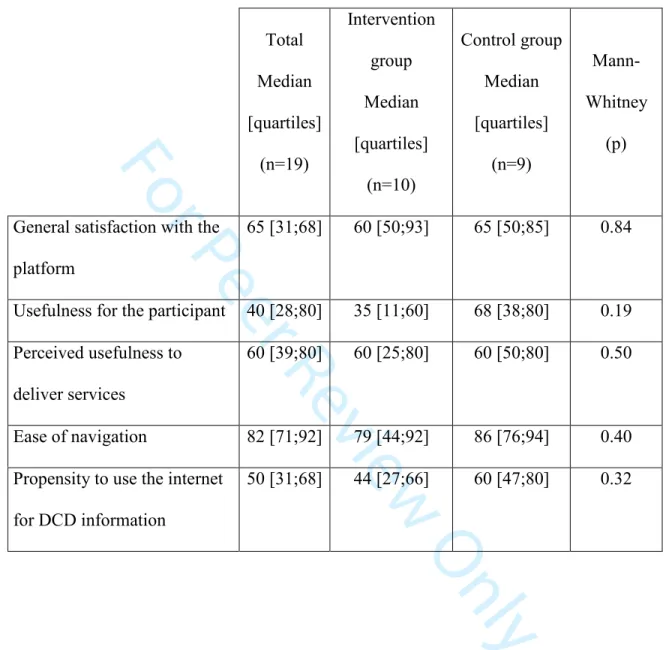
Documents relatifs
ADI: Adolescent Diagnostic Interview; CBCL: Child Behavior Checklist; CBT: cog- nitive-behavioural therapy; CTRADA: Center for Treatment Research on Adoles- cent Drug Abuse; FES:
While a recent line of research on Bayesian randomized algorithms (e.g. Thompson Sampling) has provided Bayes risk upper bounds in quite general settings ([ 35 , 34 ]), to the best
studied, using historical data or monitoring: the linear (21 km) of two small streams (“La Ligoire”) and the Louroux lake catchment. Most of those two catchments are
The aim of this study was to gain a better understanding of handwriting dysfluency by examining the accuracy and consistency of letter production both within and across
Figure1: Box plots representing maximum amplitude percentage (MA%) in children with reported motor problems (grey boxes) and age-matched typically developing children (white
(Color online) Plot of (a) s-d hybridization index for the optimized hcp and optimized icosahedral 19-atom clusters of Fe, Co, Ni, and Cu, both in the spin-polarized
/ La version de cette publication peut être l’une des suivantes : la version prépublication de l’auteur, la version acceptée du manuscrit ou la version de l’éditeur. For
The 4 types of integrity attacks, namely pollution, physical, cognitive model exploitation and execution attacks, are presented on Fig.. 4 and detailed in the rest of